SAMU de Paris
A healthcare call center operating 24/7, responding to any request for medical assistance.
Its ambulances are manned by teams of trained personnel, and are equipped with emergency equipment for any cardiac or respiratory resuscitation.
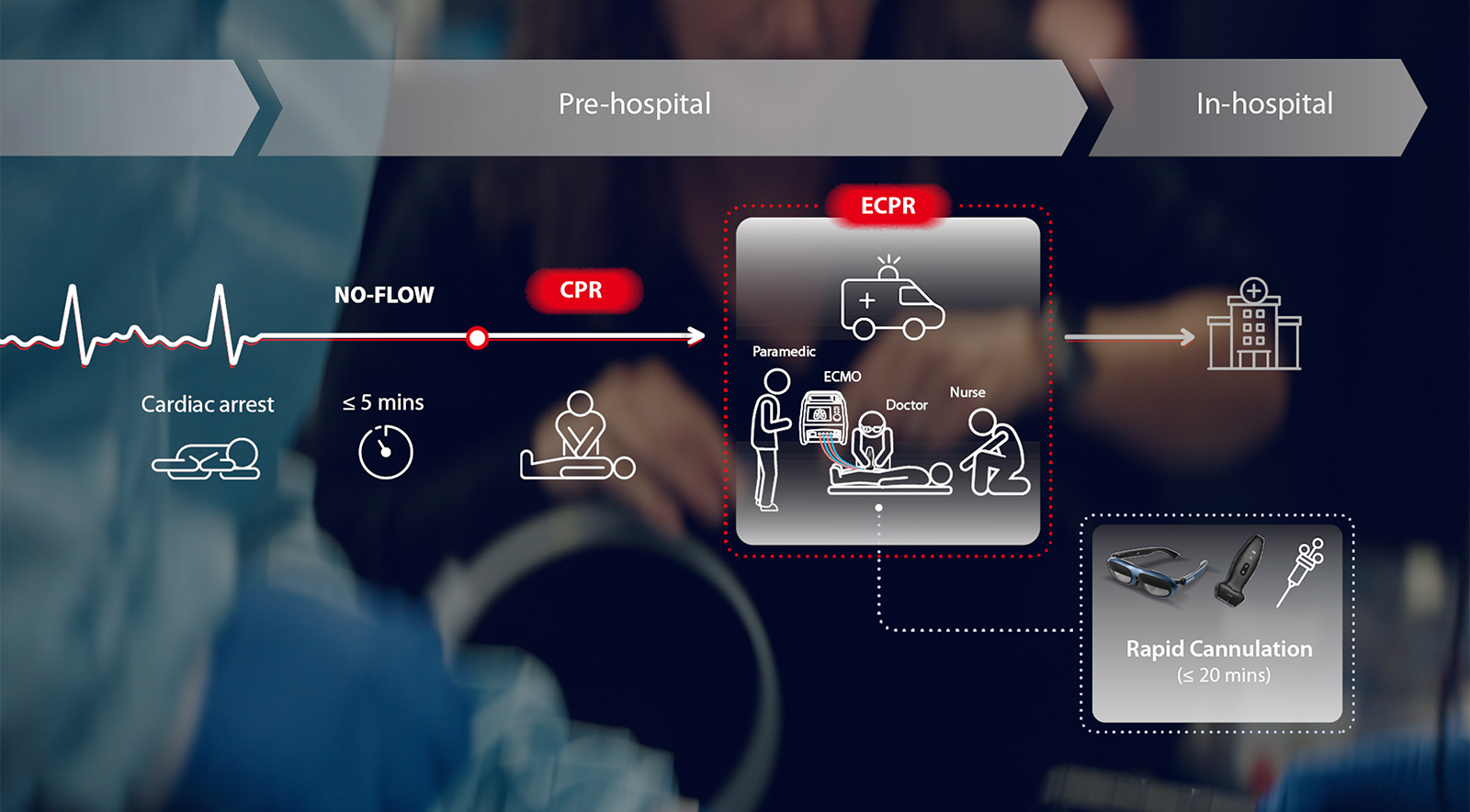
Every year, over 3.8 million out-of-hospital cardiac arrests (OHCA) occur worldwide, with a survival rate of only 8-10% (AHA). When conventional CPR fails, patients face almost certain death, especially in out-of-hospital settings where transport time consumes the narrow therapeutic window.
But what if we could enable earlier intervention? What if we could bring the most advanced life-support technology directly to the patient, rather than waiting to transport them to specialized centers?
The mobile ECPR — a revolutionary model, is maintaining end-organ perfusion whilst assessing the potential reversal of causal pathology, with the goal of improving long-term survival and neurological outcomes.
Extracorporeal cardiopulmonary resuscitation (ECPR) is a rescue therapy that takes over the function of the heart and lungs for OHCA patients. When all conventional measures, including advanced life support, have failed, ECPR is the last resort.
Although many advanced hospitals worldwide are capable of performing ECPR, only a few have taken this capability beyond hospital walls. SAMU de Paris stands out as one of the world's earliest and most specialized mobile ECPR teams—bringing extracorporeal life support directly to the scene. By coordinating expert personnel and critical equipment in real time, SAMU transforms cardiac arrest rescue into a race against time with a higher chance of survival.

A healthcare call center operating 24/7, responding to any request for medical assistance.
Its ambulances are manned by teams of trained personnel, and are equipped with emergency equipment for any cardiac or respiratory resuscitation.
In those critical moments when the heart stops beating, time becomes the enemy—every minute without proper circulation reduces the chance of survival by 7-10% (AHA).
Lionel Lamhaut MD, PhD.
Professor of EM at Paris Descartes university
Head of the ECMO Team in Paris
Associate medical director of the "SAMU de Paris"
Out-of-hospital ECPR is really a game-changer --- just like a mobile ICU. The difference between in or out-of-hospital ECPR is the delay, this is really a run. If we win time, we win life.
A 30-year-old woman, just two weeks postpartum, suffers sudden cardiac arrest.
Traditional protocols dictate transport to hospital while CPR continues — a journey that could take 20-30 minutes or more. Instead, within minutes of the emergency call, SAMU team arrives at her doorstep.
This is not just an ambulance. It's a fully-equipped mobile ICU staffed with a doctor, nurse, and paramedic specially trained in ECPR deployment. Within the critical golden hour, they assess the brain and establish ECPR circulation, then stabilize the patient for transport.
"We have patients who experienced over 60 minutes of cardiac arrest and survived," Prof. Lamhaut said. "Alive means they were able to return home to their families and resume their lives."
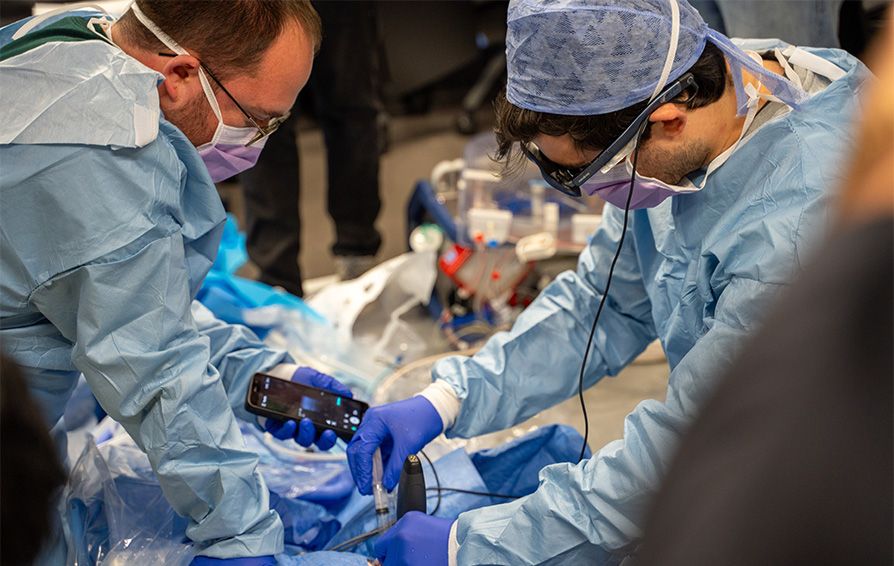
The difference between success and failure in ECMO deployment often comes down to millimeters. Cannulation—the process of inserting cannula into major blood vessels to connect the ECMO circuit—is one of the most technically challenging procedures in emergency medicine, especially when performed in the chaotic environment of a cardiac arrest scene.
"The major complication, to be short, is when cannulas are not in the artery and vein, but the cannula is in the wrong vessel," explains Prof. Lamhaut, "everything can succeed or fail by one millimeter."
This is where Mindray's wireless handheld ultrasound system TE Air and Air Realm glasses become not just helpful, but lifesaving. The portable ultrasound is pocket-sized, yet capable of providing the detailed vascular imaging needed for rapid and precise cannulation.
"With TE Air and AR glasses, we can visualize the puncture site in real time—without changing the position." said Prof. Lamhaut. "More procedures are correctly done with the glasses, and that means we have more lives saved."
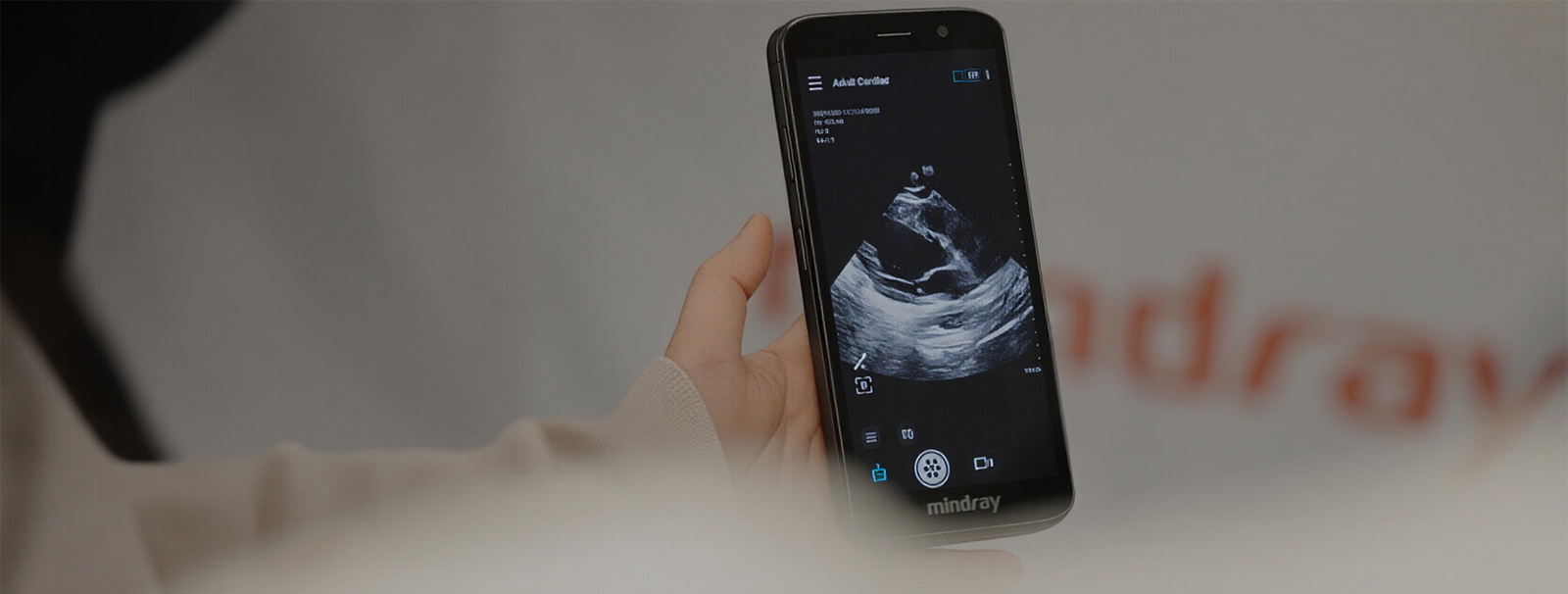
MiCo+ provides a series of dedicated applications on variable platform for different clinical scenarios, such as telemedicine and online education.
The entire SAMU team can view ultrasound images at the same time through MiCo+, enabling remote guidance and collaborative decision-making.
Today, the SAMU ECPR model has been successfully rolled out worldwide, proving its worth across France, Spain, Italy, UK, North and South America, Asia, and Australia.
Each program adapts the core principles to local healthcare systems, but the fundamental insight remains consistent: bringing advanced life support technology to the patient, rather than transporting the patient to the technology.

In 2025, SAMU ambulances raced through the city's arteries day after day, covering a 100 km radius around Paris and performing 80 pre-hospital ECMO missions with a 38% survival rate.