A Practical Guide to Guided Ultrasound Protocols for Point of Care (POC)
04-21-2026
In clinical settings, precision and speed are crucial. Guided ultrasound protocols offer a clear, systematic approach to point of care ultrasound (POCUS) exams. They can help clinicians make more accurate diagnoses quickly, which is essential when a patient is experiencing a life-threatening condition and every second counts. RUSH, eFAST, and BLUE ultrasound protocols are the three main instructional frameworks.
Explore the practical applications of RUSH, eFAST, and BLUE protocols and how they can enhance diagnostic capabilities and improve patient outcomes.
Supporting Diagnoses With Standardized Protocols
Using guided ultrasound protocols results in a more consistent, comprehensive POCUS exam. In emergency and critical care settings, clinicians need immediate, accurate insights into a patient's condition to make quick decisions about diagnosis and treatment options. By adopting these protocols, clinical teams can help improve patient safety.
eFAST, RUSH, and BLUE can reduce diagnostic variability among different users, helping to minimize subjective interpretation. Most importantly, they ensure all critical structures of the POCUS exam are properly assessed, thereby improving patient outcomes. Adopting these protocols can lower the likelihood of an incomplete exam — they can potentially spot critical pathologies and help reduce the risk of complications.
In addition, guided ultrasound protocols represent a consistent way to train clinicians, and they can be used by both new and experienced practitioners. The clear and predefined steps can also become cognitive aids under pressure, which is essential in an emergency. Common, life-threatening conditions can be addressed more quickly and with greater diagnostic confidence, elevating the quality of care.
The eFAST Ultrasound Protocol for Trauma Management
The Extended Focused Assessment with Sonography in Trauma, or the eFAST exam, uses ultrasound imaging to examine a patient's heart, lungs, and abdomen. The purpose is to quickly identify life-threatening conditions in a trauma patient. For instance, it helps detect peritoneal fluid, pneumothorax, pericardial fluid, and hemothorax (blood collection in the space between the lungs and chest) in trauma patients.
eFAST guides clinicians through many standard views:
- Pericardial (subxiphoid) view: Assesses for a pericardial effusion, which can lead to cardiac tamponade
- Right upper quadrant (Morison's pouch) view: Scanned to identify fluid between the liver and the kidney
- Left upper quadrant view: Looks for fluid between the spleen and kidney
- Suprapubic view: Checks for fluid in the pelvis
- Anterior thoracic views: Crucial for detecting pneumothorax, a collapsed lung — a common and potentially life-threatening complication in trauma
Rapidly identifying even small amounts of free fluid or air in these regions can be crucial. Clinicians get the immediate information they need to take action, speeding up the decision process to treatment.
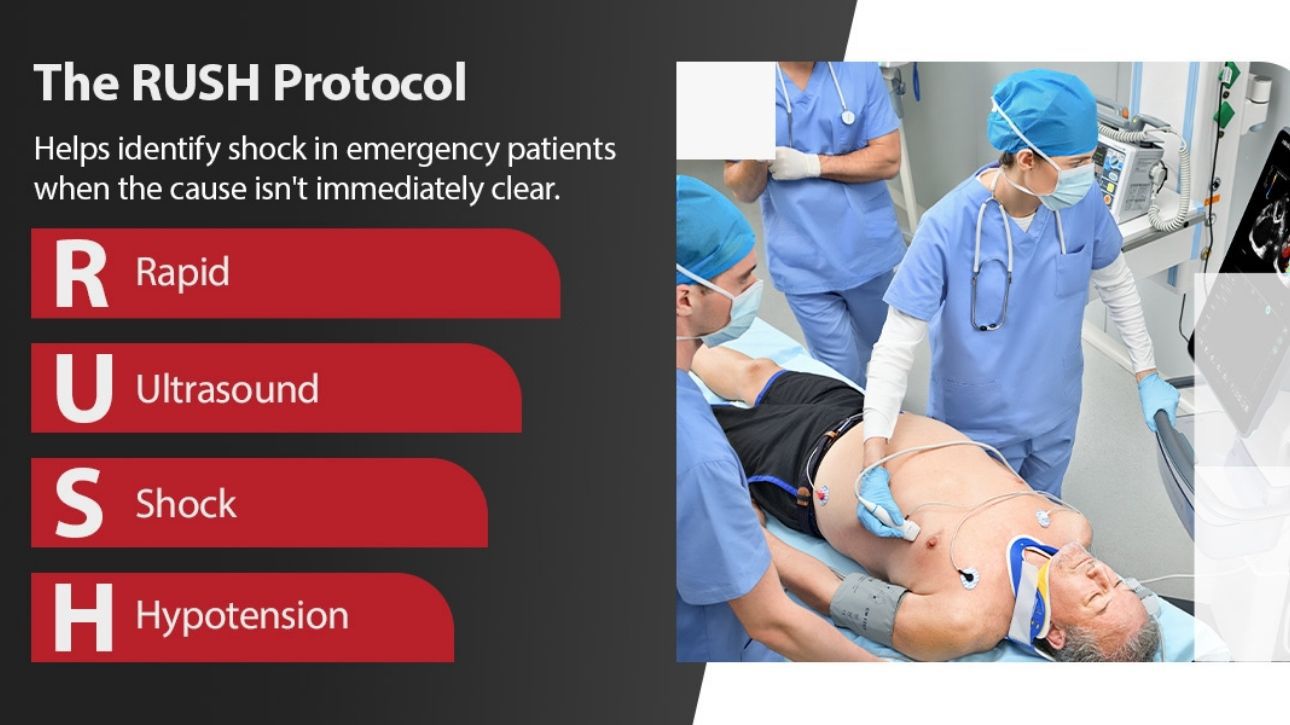
The RUSH Protocol Ultrasound for Undifferentiated Shock
The RUSH exam, which stands for Rapid Ultrasound for Shock and Hypotension, helps identify shock in emergency patients when the cause isn't immediately clear. Clinical teams can then take appropriate measures to save the patient's life. The initial RUSH protocol looks at the following major areas:
- The pump, or the heart: The pump refers to evaluation of cardiac contractility, looking for signs of right heart strain and identifying pericardial tamponade
- The tank, or the intravascular volume (IVC): This involves examining the IVC to estimate a patient's fluid status. More specifically, clinicians look at the diameter and collapsibility of the IVC to find fluid and estimate responsiveness
- The pipes, or major arteries and veins: This includes searching for major vascular issues, such as an abdominal aortic aneurysm (AAA) or deep vein thrombosis (DVT). Clinicians can quickly look for these critical vascular pathologies to make immediate decisions about their management
The BLUE Ultrasound Protocol for Respiratory Distress
The BLUE protocol, or Bedside Lung Ultrasound in Emergency, is performed to detect respiratory failure at the bedside. Timing may vary depending on the clinical situation. Clinicians use it to identify the cause of respiratory failure, looking for the following key sonographic signs:
- A-lines: These horizontal reverberations reveal a normal and dry lung surface. They suggest that there is no significant interstitial fluid
- B-lines: Often described as "lung rockets," these vertical artifacts suggest the presence of interstitial fluid commonly seen in pulmonary edema or interstitial lung disease
- Lung sliding: BLUE looks for lung sliding or lack thereof to diagnose pneumothorax
- Consolidations: These appear as tissue-like patterns and can mean fluid or inflammatory processes occurring in the lung parenchyma. Consolidations are often suggestive of pneumonia or other chronic lung diseases.
By rapidly interpreting these sonographic signs using the BLUE protocol, clinicians can spot differences between etiologies of respiratory distress. For instance, they can determine if the patient is experiencing pulmonary edema, pneumonia, or pneumothorax, helping them take the correct therapeutic interventions as quickly as possible.
Integrating Guided Protocols Into Clinical Workflows
Integrating an ultrasound machine with a guided workflow can help clinicians recognize abnormalities more clearly and quickly. Additionally, features that automate exam steps based on user-defined protocols can reduce the risk of an incomplete exam, resulting in more efficient quality assurance reviews.
Whether these advanced machines are used for automatic image annotation, activating modes, or measurement packages, the detailed guidance from these guided protocols can provide numerous benefits:
- Improve training consistency: Integrating guided protocols into your practice can lead to more consistent training for new clinicians and residents. It can ensure that everyone learns and practices the same high-quality POCUS techniques
- Streamline departmental workflow: Guided ultrasound protocols can improve clarity and help avoid confusion, leading to more efficient workflows in emergency situations
- Simplify quality assurance: From an administrative perspective, guided protocols simplify quality assurance reviews and compliance. They can address key concerns for hospital administrators and clinical leaders by demonstrating a commitment to best practices and improved outcomes
Enhance Diagnostic Capabilities With Mindray North America
To integrate these essential guided ultrasound protocols in your workflows, you need innovative technology. Mindray's Point of Care Ultrasound solutions meet the rigorous demands of emergency and critical care environments where these protocols are indispensable.
With features like advanced imaging technology, clinicians have crystal-clear visualization, while intuitive user interfaces make the systems easy to use, even under pressure. AI-powered assistive tools can further enhance diagnostic confidence and are valuable in upholding standardization across facilities, which increases efficiency and reproducibility.
Contact us to learn more about our solutions or request a quote or demo today.